
“The results from both epidemiological and physiological studies have demonstrated a strong association between excess abdominal adipose tissue and the presence of metabolic risk factors for coronary heart disease (CHD), including insulin resistance, impaired glucose tolerance, type 2 diabetes, dyslipidemia, and increased circulating inflammatory proteins”(1).
Metabolic syndrome is the name for a group of risk factors that raises your risk for heart disease and other health problems, such as diabetes and stroke.
The term “metabolic” refers to the biochemical process involved in the body’s normal functioning. Risk factors are traits, conditions, or habits that increase your chance of developing a disease.
Metabolic Risk factors (from the National Heart, Lung, Blood Institute)
The five conditions described below are metabolic risk factors. You can have any one of these risk factors by itself, but if they tend to occur together. You must have at least three metabolic risk factors to be diagnosed with metabolic syndrome.
1) A large waistline. This is also called abdominal obesity or “having an apple shape.” Excess fat in the stomach area is a greater risk factor for heart disease than excess fat in other parts of the body, such as on the hips.
2) An elevated triglyceride level (or you’re on medicine to treat high triglycerides). Triglycerides are a type of fat found in the blood.
3) A low HDL cholesterol level (or you’re on medicine to treat Low HDL cholesterol). HDL sometimes is called “good” cholesterol. This is because it helps remove cholesterol from your arteries. A low HDL cholesterol level raises your risk for heart disease.
4) High blood pressure (or you’re on medicine to treat high blood pressure). Blood pressure is the force of blood pushing against the walls of your arteries as your heart pumps blood. If this pressure rises and stays high over time, it can damage your heart and lead to plaque buildup.
5) High fasting blood sugar (or you’re on medicine to treat high blood sugar). Mildly high blood sugar may be an early sign of diabetes.
Let’s focus on a large waist line (abdominal fat). What does abdominal fat have to do with metabolic syndrome and its relation to cardiovascular disease (heart disease) i.e. how does it contribute to cardiovascular disease? Abdominal adipose tissue is not just a store of fat. Adipose tissue is very alive and is considered to act very much like an organ. It has certain metabolic processes that take place within it that produce chemicals that are detrimental to a healthy functioning body. Some of these chemical are inflammatory in-nature and can directly damage the cells that line the vessels. Abdominal adipose tissue can also release factors that cause insulin to be less affective, cause activation of the immune system to release inflammatory chemicals and increase free radical production (2-9). All of these factors are related to the damaging of the coronary vessels that supply blood and oxygen to the heart, when this happens, heart disease ensues.
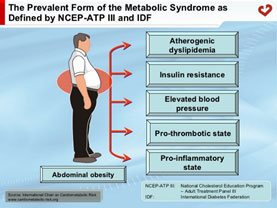
Studies show that losing abdominal fat helps lower these inflammatory chemicals and can help reduce heart disease (8, 9). Although diet is an important element in abdominal fat reduction, review of studies reveal that exercise is a crucial component to not only reduce abdominal fat but also keeping it off in the long run. Funny enough, it is not just about losing weight per se but more about losing the abdominal fat. Some studies show that people who exercised and lost fat but not weight did better than those who didn’t exercise and lost weight (10). In all, the goal is to implement an exercise regime while taking measures to loose abdominal fat through diet and lifestyle (11).
Reducing abdominal fat means decreasing a major risk factor for metabolic syndrome which in turn reduces heart and vascular disease. If you think you or someone you know may need help approaching this issue and need guidance losing weight or changing your metabolism into a healthy one give Vitalia a call and let’s get started putting you on the right track!
1) Klein, S. Is Visceral Fat Responsible for the Metabolic Abnormalities Associated With Obesity? Diabetes Care July 2010 vol. 33no. 7 1693-1694
2) Kissebah AH. Et al. : Relation of body fat distribution to metabolic complications of obesity.J Clin Endocrinol Metab 1982; 54: 254–260.
3) Bray GA, et al. The Diabetes Prevention Program Research Group. Relation of central adiposity and body mass index to the development of diabetes in the Diabetes Prevention Program. Am J Clin Nutr2008; 87: 1212–1218.
4) Klein S, et al. :Waist circumference and cardiometabolic risk: a consensus statement from Shaping America’s Health: Association for Weight Management and Obesity Prevention; NAASO, The Obesity Society; the American Society for Nutrition; and the American Diabetes Association. Am J Clin Nutr 2007; 85: 1197–202.
5) Pouliot MC, et al. : Visceral obesity in men: associations with glucose tolerance, plasma insulin, and lipoprotein levels. Diabetes 1992; 41: 826–834.
6) Banerji MA, et al. Does intra-abdominal adipose tissue in black men determine whether NIDDM is insulin-resistant or insulin-sensitive? Diabetes 1995; 44: 141–146.
7) Gastaldelli A, et al. Metabolic effects of visceral fat accumulation in type 2 diabetes. J Clin Endocrinol Metab 2002; 87: 5098–5103.
8) Fontana L, et al. Visceral fat adipokine secretion is associated with systemic inflammation in obese humans. Diabetes2007; 56: 1010–1013.
9) Fabbrini E, et al.: Intrahepatic triglyceride, not visceral fat, is associated with metabolic complications of obesity in human subjects. Proc Nat Acad Sci 2009; 106.
10) Ross, R. et al. Reduction in obesity and related comorbid conditions after diet-induced weight loss or exercise-induced weight loss in men. A randomized, controlled trial. Ann Intern Med. 2000 Jul 18;133(2):92-103.
11) Washburn, RA. Et al. Does the method of weight loss effect long-term changes in weight, body composition or chronic disease risk factors in overweight or obese adults? A systematic review. PLoS One. 2014 Oct 15;9(10):e109849.
12) Johns, DJ., et al. Diet or exercise interventions vs combined behavioral weight management programs: a systematic review and meta-analysis of direct comparisons. J Acad Nutr Diet. 2014 Oct;114(10):1557-68.
13) Franz, MJ., et al. Lifestyle weight-loss intervention outcomes in overweight and obese adults with type 2 diabetes: a systematic review and meta-analysis of randomized clinical trials. J Acad Nutr Diet. 2015 Sep;115(9):1447-63.
14) Emadian, A. et al. The effect of macronutrients on glycaemic control: a systematic review of dietary randomised controlled trials in overweight and obese adults with type 2 diabetes in which there was no difference in weight loss between treatment groups. Br J Nutr. 2015 Nov 28;114(10):1656-66.
By
Dr. Quinn Rivet B.Sc., N.D.


