September is PCOS awareness month. PCOS is often a lifelong condition that can have grievous mental and physical symptoms including:
- Irregular or absent periods
- Cystic Acne
- Infertility
- Hirsutism
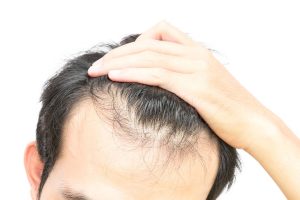
- Hair loss
- Insulin resistance leading to diabetes and or metabolic syndrome
- Depression
Hair loss associated with PCOS is now recognized as androgenic alopecia or female pattern hair loss. This pattern of hair loss is often seen as diffuse thinning along the front and vertex. While hair loss can range from mild to severe, bald areas are not typically seen.
This androgenic hair loss results from an increase of androgen hormones; Testosterone and DHEA. While these are commonly known as male hormones, Testosterone and DHEA are present in all women in low levels.
It is now recognized with a growing body of research that insulin resistance and defects in insulin signaling pathways are the main driver behind PCOS (1). This insulin resistance is also the main driver for the elevated androgens by signaling the ovaries to produce more testosterone (2,3).
Diet, exercise and stress management are the foundation for supporting PCOS (4). Weight loss is indicated with elevated BMI (3). In lean PCOS, where we see a healthy BMI, there is still often insulin resistance. Insulin resistance occurs in 70-95% of people with obese PCOS and 30-75% of people with lean PCOS (2,5)
Pharmaceutical or nutraceutical intervention is often indicated beyond diet and lifestyle. Unfortunately historically when a younger women presented with irregular periods, they were often put on an oral contraceptive as a solution. Oral contraceptives do not treat the underlying insulin resistance or the elevated androgens. In fact certain OCPs can increase androgens and it is debated if OCP can actually worsen insulin resistance (6).
Hair loss is detrimental at any age. Finding the cause and the correcting the imbalance is always the first step to restoration.
Elizabeth Miller, ND
1.Baptiste CG, Battista MC, Trottier A, Baillargeon JP. Insulin and hyperandrogenism in women with polycystic ovary syndrome. J Steroid Biochem Mol Biol. 2010;122(1-3):42-52. doi:10.1016/j.jsbmb.2009.12.010
2.Marshall JC, Dunaif A. Should all women with PCOS be treated for insulin resistance?. Fertil Steril. 2012;97(1):18-22. doi:10.1016/j.fertnstert.2011.11.036
3.Nestler JE, Jakubowicz DJ, de Vargas AF, Brik C, Quintero N, Medina F. Insulin stimulates testosterone biosynthesis by human thecal cells from women with polycystic ovary syndrome by activating its own receptor and using inositolglycan mediators as the signal transduction system. J Clin Endocrinol Metab. 1998 Jun;83(6):2001-5
4. International evidence-based guideline for the assessment and management of Polycystic Ovary Syndrome (PCOS). https://www.monash.edu/medicine/sphpm/mchri/pcos/guideline
5.Stepto, N.K., et al., Women with polycystic ovary syndrome have intrinsic insulin resistance on euglycaemichyperinsulaemic clamp. Hum Reprod, 2013. 28(3): p. 777-84.
6. Diamanti-Kandarakis E, Baillargeon JP, Iuorno MJ, Jakubowicz DJ, Nestler JE. A modern medical quandary: polycystic ovary syndrome, insulin resistance, and oral contraceptive pills. J Clin Endocrinol Metab. 2003 May;88(5):1927-32